Are statin drugs doing more harm than good?
It is important to weigh the risks versus the benefits of any medication before taking it. Statins, the most widely prescribed class of cholesterol medications, have been scrutinized by the media on several occasions . . . causing patients to question whether these medications do more harm than good. However, they have an enormous amount of “outcome” data, proving they do more than just lower cholesterol; they decrease heart attacks and strokes. So why all the controversy? Let’s take a deeper look at the data we have on statins, and address some these questions and concerns.
Will statins cause diabetes?
According to the American Heart Association (AHA), “The risk of statin-induced newly diagnosed diabetes is about 0.2% per year.” (REF 1)
In a meta-analysis of 13 different statin trials (evaluating over 90,000 patients), the data concluded you would have to treat 225 patients with statins for four years to get one extra case of diabetes (REF 2). In the Jupiter trial, there was a small increase (one tenth of a point) seen in Ha1c (a lab test that represents a three month average of blood sugars), but glucose levels never went up. This 0.1 increase in Ha1c could possibly push someone from a value of 6.4 to 6.5 (which would then warrant a diagnosis of diabetes) . . . but statins will not cause people with normal glucose metabolism to suddenly become diabetics!
It is also important to note that there is lab variability with the Ha1c test, so a 0.1 difference could occur even the same day if the patient's same blood was run two different times at the lab. Researchers at Harvard Medical School published the findings of their study in the journal Science Translational Medicine that indicated the accuracy of the HbA1c test depends on the age of a individual's red blood cells. The HbA1c test measures the extent to which glucose has become attached to a protein in red blood cells, so if one person has red blood cells that live slightly longer than another person’s, that first individual will have a higher HbA1c level . . . even if both people have the same average blood glucose level. (REF 26)
In a different pooled analysis of data from 5 statin trials (evaluating over 30,000 patients), they found that high-dose statin therapy was more associated with an increased risk of new-onset diabetes than moderate-dose statin therapy. For every 498 patients treated with high-dose therapy, there was one new case of diabetes. However, even with high-dose statin therapy, you would only need to treat 155 patients to decrease one cardiovascular event (REF 3). And clearly, the benefits of reducing coronary events outweigh the potential risk of developing diabetes. But even this small risk of developing diabetes can be minimized by taking a lower dose statin, and by avoiding certain brands of statin drugs. In a study of around 9,000 people, Atorvastatin (Lipitor) and Simvastatin (Zocor) conveyed the highest risk of diabetes; the other statins did not show this same increased risk. (REF 4)
However, for those patients who are still concerned about this small risk, there are advanced blood tests that can identify a patient’s risk of diabetes years before their blood sugars rise . . . so any potential risk can be mitigated with proper diet and/or medication.
Will statins cause memory loss?

The FDA warns that some people have developed memory loss or confusion while taking statins, but that these side effects reverse after discontinuing the medication (which is very different from dementia). However, as the AHA statement enforced, “There is no convincing evidence for a causal relationship between statins and cognitive dysfunction.” (REF 1, REF 6) In actuality, there has been evidence that statins may help with brain function!
One study of over 1,600 people showed a 48% decrease in the incidence of dementia in the patients who took statins (REF 7). Another study of 57,000 patients showed an inverse relationship between statin use and dementia (REF 8). A third study of over 400 thousand statin users showed a 20 – 25% reduced risk of Alzheimers disease (REF 9). And yet another study demonstrated a 50 % reduced dementia risk in patients with atrial fibrillation who took statins (REF 10).
Will statins help with inflammation?
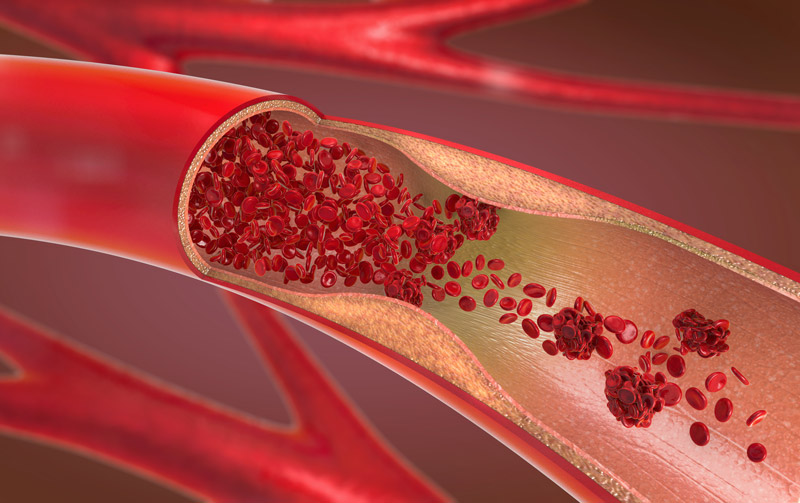
Statin medications function like anti-inflammatory medications for your arteries.
Inflammation is the main driving factor in both heart disease and Alzheimers . . . and statins decrease arterial inflammation. The Jupiter Trial was proof of this. In a collaborative effort involving 1315 physicians in 26 countries (and nearly 18,000 patients), the Jupiter Trial evaluated patients with normal cholesterol levels (LDL-C < 130) but elevated arterial inflammation (hsCRP levels > 2). These patients were found to greatly benefit from statin therapy . . . so much so that the study was stopped early (after 1.9 years instead of 5). (REF 5). In the statin-treated population, there was a 54% reduction in heart attacks, a 48% reduction in stroke, and a 46% reduction in need for arterial revascularization (all in patients who, according to current lipid guidelines and known risk factors, were considered to be “low risk” and not candidates for statin therapy). So clearly, there are non-lipid benefits to statins beyond just lowering cholesterol!
“Of the nearly 1.7 million heart attacks and strokes that occur annually in the United States, more than half occur among apparently healthy men and women with average or low levels of cholesterol.” (REF 11) This is why inflammatory biomarkers are so important to test in patients. One of those biomarkers is hsCRP, which was shown to independently predict CV events in women better than LDL cholesterol (REF 12).
Will statins cause my muscles to ache?

Compared to placebo, the actual risk of developing muscle pain as a result of taking a statin is about 5 percent or less, and it was seen more with Atorvastatin (Lipitor) than other statins (REF 13).
Very rarely, statins can cause life-threatening muscle damage called rhabdomyolysis, which can be severely painful. Rhabdomyolysis can occur when you take statins in combination with certain drugs, or if you take a high dose of statins. The actual risk of this very serious side effect is extremely low, calculated to occur in only a few cases per million people taking statins. According to the AHA, “The risk of statin-induced serious muscle injury, including rhabdomyolysis, is <0.1%, and the risk of serious hepatoxicity (liver damage) is about .001%.” (REF 1)
For those who are still concerned, there is a genetic test called the “statin myopathy” test (SloCo1b1) that can determine how an individual metabolizes statin medications. A person can carry one or two copies of this gene, and if they do, they are at increased risk of having muscles aches when taking a statin (REF 14, REF 17), particularly when taking fat-soluble statins (like Lipitor and Zocor). In patients with the SloCo1b1 gene, prescribing water-soluble statins (like Crestor, Livalo, or Pravachol) will help improve tolerability.
How can I minimize side effects from a statin?

For those patients who experience side effects on a statin, there are a few things that might help. (READ MORE HERE). Raising coenzyme Q10 and vitamin D levels can lessen myalgias for many patients. Using water-soluble statins can also minimize side effects (especially in those with the SloCo1B1 gene).
Crestor (rosuvastatin) is my preferred statin because it is an affordable option that is often better tolerated than Lipitor (atorvastatin) and Zocor (simvastatin). In addition, Crestor has been shown to be better at decreasing arterial inflammation and raising HDL (good cholesterol) than other statins. It can also be an effective treatment for patients no matter what their genetic make-up (Kif6). For those who cannot tolerate Crestor, I often use Livalo (pitavastatin). Livalo is metabolized through multiple pathways, so often tolerated even when other statins are not. In highly sensitive patients, even a small dose taken every other day can improve lipids and lower CV risk. If after all these efforts the patient still cannot tolerate a statin, then a PCSK9 inhibitor may be the best medication for them.
Can you lower cholesterol levels too much?

Cholesterol is a fatty substance produced by the liver to help the body perform many different functions, including forming cell membranes (a key building block for our hormones and our nerve and brain function). Some have speculated since this is the case, more cholesterol must be better, but this has not been proven.
The blood-brain barrier is actually impermeable to circulatory cholesterol, so cholesterol regulation in the brain is not similar to that of extra-cerebral cholesterol (meaning cholesterol levels outside of the brain should not affect brain function, as these two cholesterol pools are different). (REF 23).
Studies have actually shown that the lower the LDL cholesterol, the lower the CV risk (lower than 70 is ideal, but lower than 54 may be even better.) (REF 20). The normal low-density lipoprotein (LDL) cholesterol range is 50 to 70 mg/dl for native hunter-gatherers, healthy human neonates, free-living primates, and other wild mammals . . . all of whom do not develop atherosclerosis (plaque in their arteries). (REF 27) A newborn baby (who carries high developmental demands) has an average LDL of only 35 mg/dL, so this small amount of cholesterol appears to be sufficient to maintain vital cellular functions (REF 22). Furthermore, studies evaluating PCSK9 inhibitors (a class of cholesterol medications that can drop cholesterol extremely low) found that very low cholesterol levels did not adversely affect the patients.
Is high dose statin therapy better than low dose?
High dose statins are superior for patients with acute or substantial arterial inflammation, like patients who have had a recent heart attack. This was shown in the A to Z trial and in the Prove It trial (REF 16). However, the 2008 SEARCH trial (the largest and longest trial looking at high dose versus low dose statin therapy) showed that high dose statin therapy was not superior to low dose for lowering major vascular events and all-cause mortality . . . in patients with stable heart disease (REF 18). So once inflammation stabilizes, it seems reasonable to decrease the statin dose (especially since potential side effects and complications are often dose-dependent).
The current cholesterol guidelines recommend all patients with CV risk receive a high-dose statin in order to lower LDL-C more than 50%. (REF 25) However, we have the capability of doing specialized blood work (Cholesterol Balance Test) to determine the real source of each patient’s cholesterol problem (whether the liver is producing too much cholesterol, or the intestines are simply absorbing too much). Doubling the dose of a statin only offers an additional 5-10% lowering in LDL cholesterol (REF 19), so instead of prescribing a high-dose statin and increasing the risk of potential side effects, we often prescribe low-dose statins and then add on Zetia (ezetimibe) if needed. Zetia is a non-statin, well-tolerated medication that can further lower cholesterol by shutting down the absorption of cholesterol in the intestines (IF the results of the cholesterol balance test indicate this would be beneficial). In the IMPROVE-IT trial, Zetia lowered cardiovascular events when added onto statin therapy (REF 20), so we have “outcome” data to back it up. This trial also indicated that the lower the LDL cholesterol, the better (A LDL-C of 53 was superior to a LDL-C of 70). (REF 24)
In conclusion . . .

There are several ways to determine a patient’s cardiovascular risk beyond the standard lipid panel. Blood tests that evaluate arterial inflammation, and other testing like CPET, CIMT, or CACS that look directly at vascular health, can all help identify whether a patient has plaque build up (atherosclerosis) and whether that plaque could be at risk of rupturing and leading to a blood clot (which could cause a sudden heart attack or stroke . . . even in patients who have recently passed a stress test with a cardiologist).
At Whole Heart Family Medicine, we do not necessarily recommend patients take a statin if their only identified risk factor is elevated cholesterol, but we are very aggressive treating patients with elevated inflammation markers or existing atherosclerosis. Even the 2018 ACC/AHA guidelines on cholesterol management favor treating patients with a coronary artery calcium (CACS) score of only 1 (any documented plaque) with statin therapy. (REF 21)
In the end, we agree with the American Heart Association's stance - “In patients with cardiovascular (CV) risk, statin treatment should be delivered as the benefits greatly outweigh the risks.” (REF 1) Any patient with documented atherosclerosis (plaque in their arteries) carries CV risk . . . and those with arterial inflammation are also at increased risk.
When a patient’s individual genetics and vitamin deficiencies are properly addressed, and the appropriate medication (and dosage) are chosen, there are many ways to maximize the benefit of this class of medications while minimizing potential side effects.
REFERENCES
1 – https://professional.heart.org/professional/ScienceNews/UCM_503181_AHAs-Statement-on-the-Safety-Profile-of-Statins-Big-Benefit-with-Low-Risk.jsp
2 – https://www.ncbi.nlm.nih.gov/pubmed/?term=sattar%2C+preiss%2Cstatins%2C+diabetes%2C+2010
3 - https://www.ncbi.nlm.nih.gov/pubmed/21693744
4 – https://www.ncbi.nlm.nih.gov/pubmed/25754552
5 – https://www.ncbi.nlm.nih.gov/pubmed/18997196
6 – https://www.ncbi.nlm.nih.gov/pubmed/18199831
7 - https://www.ncbi.nlm.nih.gov/pubmed/?term=cramer+neurology+2008+use+of+statins+and+incidence+of+dementia
8 - https://academic.oup.com/eurheartj/article/34/suppl_1/1609/2860097
9 – https://www.ncbi.nlm.nih.gov/pubmed/?term=zissimopoulos+sex+and+race+differences+in+the+association+between+statin+use+and+the+incidence+of+alzheimers
10 - https://www.ncbi.nlm.nih.gov/pubmed/26080283
11 - https://www.ahajournals.org/doi/full/10.1161/CIRCOUTCOMES.109.868299
12 - https://www.ncbi.nlm.nih.gov/pubmed/12948872
13 - https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4450764/
14 – https://bostonheartdiagnostics.com/test/boston-heart-statin-induced-myopathy-slco1b1-genotype-test/
15 – https://www.mayoclinic.org/diseases-conditions/high-blood-cholesterol/in-depth/statin-side-effects/art-20046013
16 – https://www.2minutemedicine.com/the-prove-it-trial-high-dose-statin-regimen-reduces-mortality-after-acs-classics-series/
17 – https://www.nejm.org/doi/full/10.1056/nejmoa0801936
18 – https://www.acc.org/latest-in-cardiology/clinical-trials/2010/11/10/12/01/search
19 – https://www.acc.org/latest-in-cardiology/articles/2016/03/09/06/50/ezetimibe-the-lower-the-ldlc-the-better
20 – https://www.acc.org/latest-in-cardiology/clinical-trials/2014/11/18/16/25/improve-it
21 - https://www.acc.org/latest-in-cardiology/ten-points-to-remember/2018/11/09/14/28/2018-guideline-on-management-of-blood-cholesterol
22 - https://pdfs.semanticscholar.org/5979/72ce84a6244337143e613acb147e2d1a434d.pdf
23 - https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5937425/
24 - https://www.ncbi.nlm.nih.gov/pubmed/26559810
25 - https://www.acc.org/latest-in-cardiology/ten-points-to-remember/2018/11/09/14/28/2018-guideline-on-management-of-blood-cholesterol