- Home
- About Us
- Advanced Testing
- Nutrition & Self-Care
- Further Learning
- New Member Info
- Contact
A CPET test is a stress test that assesses both heart and lung function during exercise. A CPET test can help identify existing cardiovascular (CV) or pulmonary disease, but it is different than a traditional stress test. Cardiologists perform treadmill or nuclear stress tests in attempt to identify patients with advanced blockages in their coronary arteries (severe disease that may require immediate intervention with stent placement or open bypass surgery). However, patients can pass these stress tests and still have blockages in their arteries, particularly their smaller ones. This small vessel disease leads to a gradual loss in circulation and slow loss of function . . . and eventually even heart failure and death. Furthermore, the smaller plaques (that are not completely occluding an artery) can suddenly rupture, causing a blood clot that precipitates a heart attack or stroke (which is the more common cause of a heart attack). So unlike regular stress tests, the CPET can identify cardiovascular problems at an earlier stage when only the small vessels are involved, and without exposing the patient to any radiation in the process!
Individuals with NO known risk factors can still develop heart disease. Current medical guidelines endorse using risk calculators to determine a patient’s CV risk (and to guide treatment recommendations), but they can mislabel patients as healthy who in fact have hidden risk factors or small vessel disease.
Atherosclerosis (plaque in the arteries) is a chronic disease process that starts early in life and results in diminished circulation throughout the body over time. It is the leading cause of loss in quality of life and the leading cause of death in both men and women . . . so it is critical to identify this disease early and treat it aggressively (before a heart attack, stroke, heart failure, dementia, or loss in sexual function occur).
When symptomatic patients have no identifiable coronary artery disease on a coronary angiogram, they are still at increased risk for CV events (which appears to be more common in women). 2 In many cases, an abnormal cardiac response on a CPET may be the only objective evidence of this patient’s potentially undertreated ischemic heart disease.
Any patient who experiences shortness of breath or easy fatigability with exertion would highly benefit from a CPET. However, we recommend all of our patients with cardiovascular risk factors get a baseline test. The sooner we can identify which patients have existing atherosclerosis, the sooner we can suggest medications and lifestyle changes to stop, and even reverse, the disease process.
CPET can also be a beneficial tool for pre-operative evaluation. It can more accurately identify patients who carry a higher risk for CV complications during surgery (READ MORE HERE). CPET has even been validated as an accurate tool to help assess operative risk in patients about to get bariatric surgery (READ MORE HERE).
The CPET helps to stratify the cardiac risk of each patient by assessing the presence or absence of cardiac dysfunction (even at an early stage), mainly through the assessment of peak exercise capacity.
The information gathered during a CPET is used to calculate Peak VO2 (the highest level of oxygen consumption attained at peak exercise). Peak VO2 is the best measure of cardio respiratory fitness, also known as functional capacity or exercise capacity . . . and it is the #1 predictor of longevity and all-cause mortality. The Peak VO2 indicates how much oxygen you are able to convert into energy (ATP) and actually deliver to your muscles and organs via your circulatory system.
Think of Peak VO2 like a global vital sign – one of the best markers of a patient’s overall health. It reflects the effects of chronic diseases on the aging process, and quantifies the physiological “reserve” remaining in an individual. Low levels of Peak VO2 have been linked to decreased survival from heart disease, stroke, lung disease, cancer, kidney disease . . . as well as increased incidence of hypertension, diabetes, high cholesterol, dementia, pneumonia and osteoporosis. (Read the study HERE).
The Peak VO2 goal will vary for each patient, depending on his or her age, height, weight, and sex. Individuals who achieve a Peak VO2 > 100% predicted live the longest with the fewest health problems; whereas those with Peak VO2 < 60% of predicted have the shortest survival with the most health problems . . . in a dose-dependent manner.
Another value calculated by CPET is the peak O2-pulse, which indicates how much blood one’s heart can pump out with each beat (at the peak level of exercise). This peak value tracks with the severity of underlying heart disease. If this parameter starts to decrease during late exercise, then it becomes diagnostic for the presence of small vessel disease, and confirms the need for more aggressive lifestyle and medical interventions.
If the CPET indicates a patient has inducible myocardial dysfunction (IMD), then they have undertreated atherosclerosis that is hindering the heart’s ability to deliver oxygen to their muscles and organs during exercise. Depending on the severity, these patients may experience shortness of breath, fatigue, or muscle pain when they exert themselves at higher workloads. Beta-blocker medications may benefit these patients because they can help improve exercise tolerance by increasing the peak O2-pulse.
With progression of coronary disease, peak cardiac function (Peak VO2) will deteriorate, so serial CPET testing serves as a key tool to help monitor changes in cardiac health over time. Improvements can be seen within six months of implementing lifestyle and medical therapies, but at the very minimum, patients with an abnormal CPET should have one done annually to follow the course of their disease and confirm response to therapeutic interventions.
Patients started on beta-blocker medication may need to repeat their test in one month to determine the most effective dosage for optimizing cardiac function (since this will vary among individuals).
The goal in every person is to increase Peak VO2 from baseline by 10% or more per test until the underlying cardiac dysfunction pattern is completely normalized (as seen in the case study HERE).
(Mayo Clin Proc 2018;93(1):48-55)
Both CIMT and CPET can help identify vascular disease at an early stage, but the two tests offer very different information. Ideally, all patients with risk factors, or with known atherosclerosis, should have both of these tests done annually. The information from these tests can be used synergistically to monitor progression or regression of CV disease.
Improvements in CIMT measurements should correlate with improved CPET values, but not necessarily the other way around. CPET values will start to improve as soon as the microcirculation begins to open up, whereas improvements in CIMT measurements (in the larger vessels) may take a little longer to reflect the benefit of therapeutic interventions.
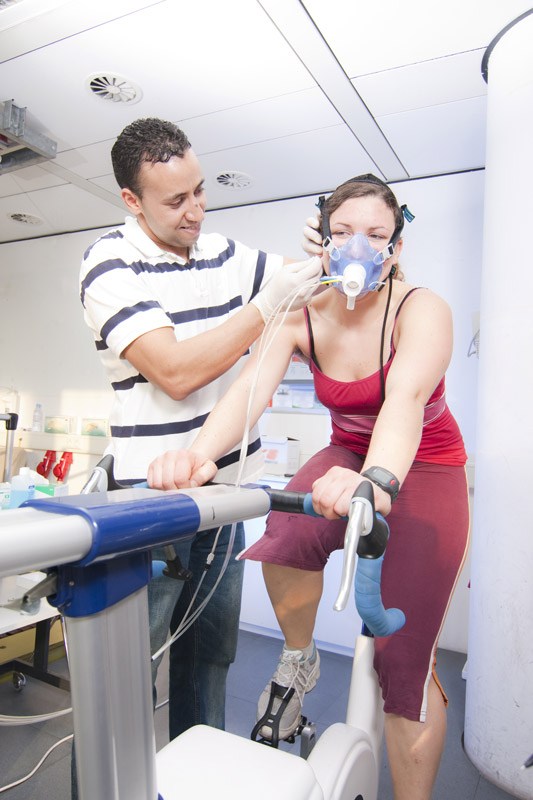
CPET testing is done on a stationary bicycle, which is safer for patients than a treadmill. A mask is placed over the mouth and nose to monitor the oxygen used, carbon dioxide produced, and breathing pattern. The mask does not restrict breathing, and the patient only breaths in room air through the test. Electrocardiogram (EKG) stickers are placed on the patient’s chest to monitor heart rate and rhythm, and a blood pressure cuff is used to measure blood pressure throughout the test. Before exercise begins, the patient performs a series of lung tests to assess pulmonary function. Once the patient is seated comfortably on the bike, they will begin to pedal lightly for a few minutes to warm up. The resistance will be increased slowly so it will get harder to pedal, as if they were going up a hill that keeps getting steeper. It is important to pedal at the same speed for the entire test, even when it is difficult.
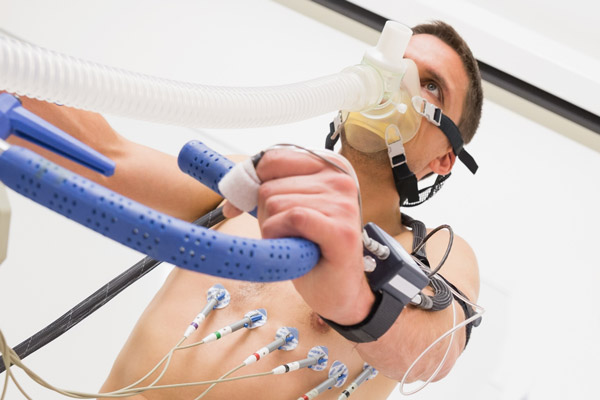
The patient should avoid speaking during the test, unless they are experiencing discomfort or pain. The test will continue until the patient is giving their maximum effort and can no longer continue. However, if the technician notices the patient is experiencing certain symptoms, the test will be immediately stopped. After the test is over, the technician will ask the patient to pedal slowly and gently cool down while they continue to monitor the patient’s vital signs.
To get the most accurate results, it is very important that the patient GIVE THEIR BEST EFFORT for as long as they possibly can. If they do not give a maximum effort, the test may be “indeterminate,” and the ordering clinician will not have the most accurate information to help the patient.
The actual time it takes to perform the bike portion of the test, from the time the patient gets on the bike, through the exercise portion and recovery, will be between 15 and 25 minutes. However, the patient will only be asked to exercise at a hard intensity for about 3 to 4 minutes.
The main therapeutic interventions are lifestyle (diet, smoking cessation, exercise) and medical (statins, angiotensin-converting enzyme inhibitors, and beta-blockers). The combination of these different therapies can improve cardiac and arterial health by opening-up the microcirculation . . . and the effectiveness of these treatments can be measured through tracking Peak VO2 measurements over time.
This is the most important factor. Patients are encouraged to exercise on a regular basis, for 30 minutes or more in their moderate heart rate zone (as individually determined by the CPET exercise prescription). Quitting smoking, weight loss, and treating sleep apnea are also key lifestyle interventions that will help improve CPET values.
This class of medications is typically prescribed for patients with high cholesterol; however, there are other CV benefits to taking a statin. Statins decrease inflammation in the arteries and stabilize arterial plaque . . . and they can improve cardiac function by reversing small vessel disease.
This class of medication is typically used to treat high blood pressure, but they have proven to offer many other CV and renal (kidney) benefits. For this reason, they are indicated for us in diabetics and in patients who have congestive heart failure or coronary artery disease. Ace Inhibitors help improve endothelial dysfunction (disease in the lining of the arteries) by opening up the microcirculation, which can help restore healthy elasticity to the arteries and cardiac muscle. 3
This class of medications is typically used to treat high blood pressure, but they offer other CV benefits (including an indication for use in patients with congestive heart failure). Beta blockers decrease one’s heart rate, and by doing so, allow the heart more time to fill with blood in-between beats (thus increasing how much blood the heart can pump out with each beat). The more blood the heart can pump out, the more oxygen it can deliver to the muscles and organs. The benefits of beta-blockers are best demonstrated by the improvements seen in Peak O2-Pulse.
CoQ10 enhances mitochondrial function (the cells ability to convert oxygen into energy) and thus improves the microcirculation. This correlates with improvements in endothelial dysfunction, and improved CPET performance in patients with coronary disease and heart failure.
This supplement benefits patients with small vessel disease the most (not patients with established large vessel coronary artery disease). Studies have demonstrated improved coronary blood flow in patients who took L-arginine for six months. 4 Because of its short half-life, L-Arginine is most effective if three grams is taken three times a day (preferably with L-Citrulline for better absorption).
This medication increases the force with which the heart contracts, so it increases the Peak O2-Pulse. It can be helpful for patients who are symptomatic from small or large vessel disease (patients who experience chest pain or shortness of breath with exertion due to cardiovascular disease). Taking Ranexa may help this patient tolerate exercise, which is ultimately the best thing for improving CV health over time.
*Medical articles and research related to CPET (READ MORE HERE)
*You can learn more about CPET testing at www.mymettest.com
Do something today for a better tomorrow!
Make an appointment now for advanced testing. We are here to help.
REFERENCES
1 – A practical clinical approach to utilize cardiopulmonary exercise testing in the evaluation and management of coronary artery disease: a primer for cardiologists - Copyright - 2017 The Author(s). Published by Wolters Kluwer Health, Inc.
2 – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3018605/
3 - https://jamanetwork.com/journals/jamainternalmedicine/fullarticle/410089